OVERVIEW on ...
HOW Dry Eye Disease GETS WORSE
CONSEQUENCES of BASIC CAUSATIVE FACTORS are PRIMARY PATHOLOGY of the Tear FILM and Ocular SURFACE
The main PRIMARY Pathologies in Dry Eye Disease are Tear Film Deficiency and Ocular Surface Tissue Damage.
The main PRIMARY Pathologies in Dry Eye Disease are Tear Film Deficiency and Ocular Surface Tissue Damage.
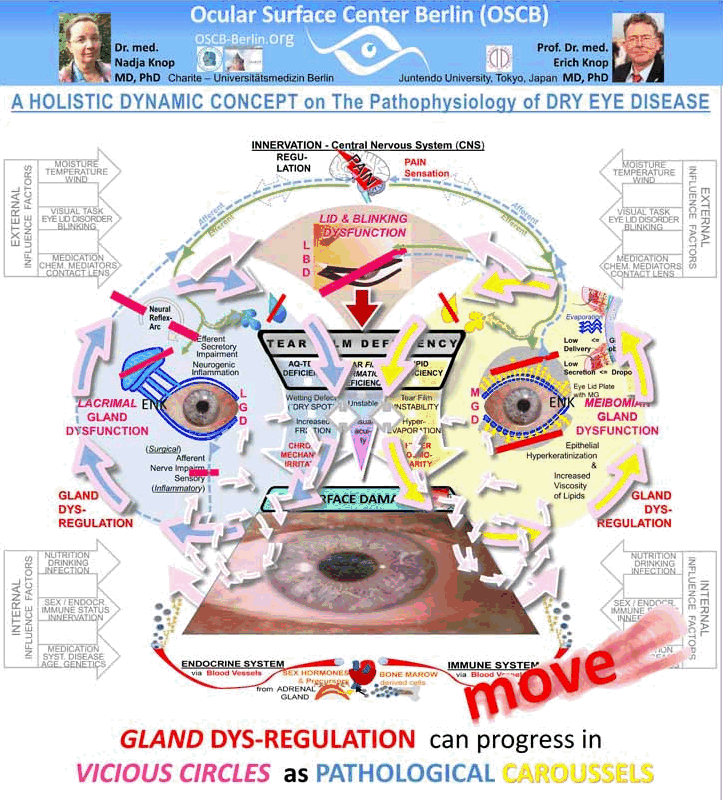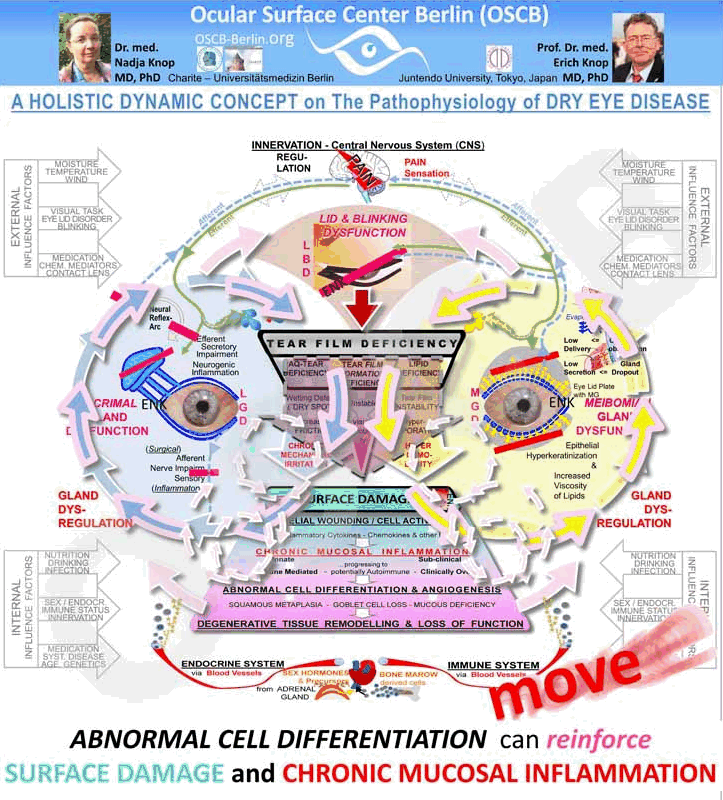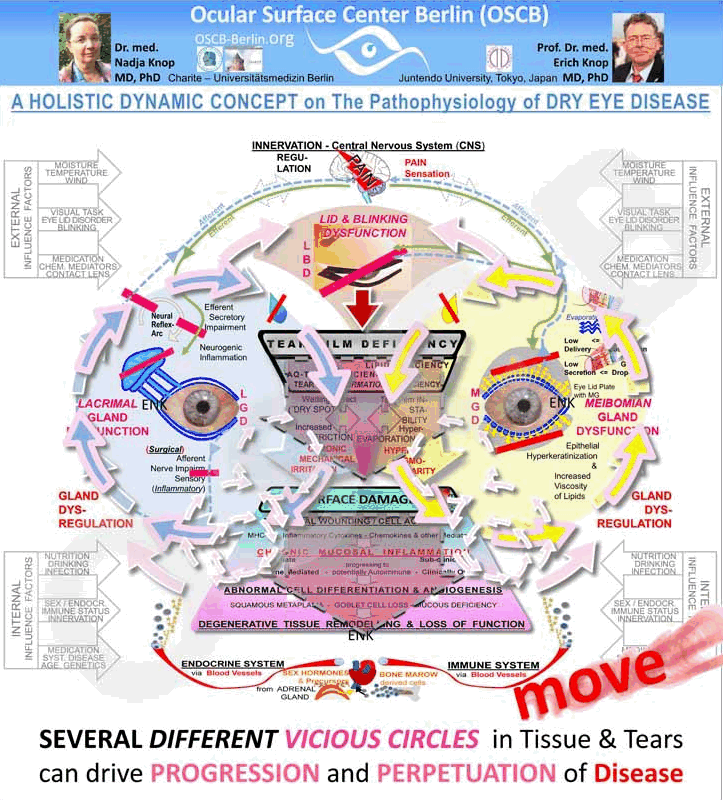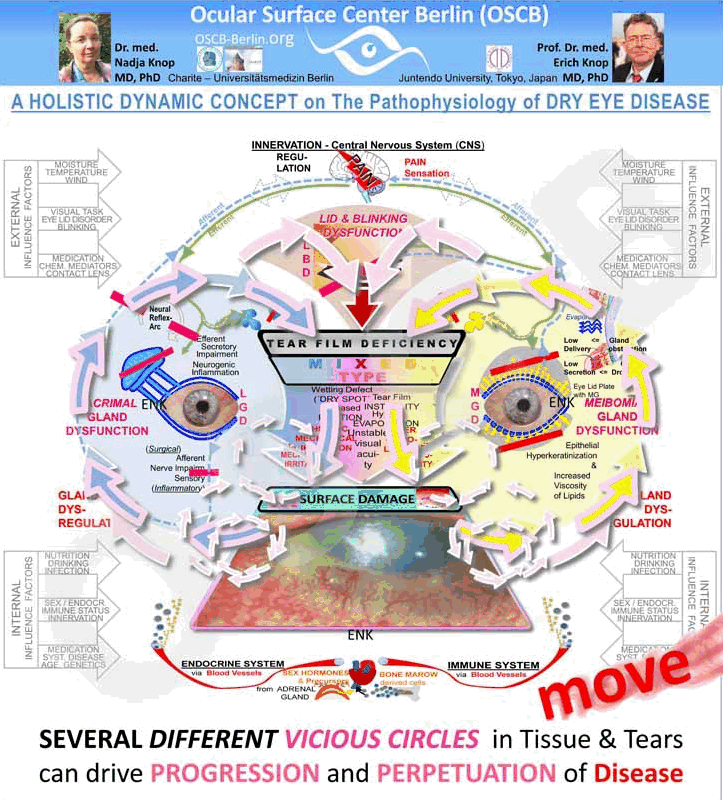
When a dysfunction of gland SECRETION of at least one component - mucins, water or lipids - of the tear film occurs, this leads to Pathology of the Tear Film - termed TEAR FILM DEFICIENCY. This is a PRIMARY Pathology of Dry Eye Disease.
When Tear Film Deficiency exists, this gives rise to sequences of various SECONDARY Pathogenetic Factors such as
Instability of the tear film with
early Break-Up of the tear film and the
formation of Dry Spots at the Ocular Surface.
etc. please see the diagram to the right
SECONDARY PATHOGENETIC FACTORS IN TEAR DEFICIENCY LEAD TO MECHANICAL FRICTION AND HYPER-OSMOLARITY OF TEARS.
Tear Film Deficiency typically leads to Damage of the Ocular Surface. This occurs via Sequences of Secondary Pathogenetic Factors in the tear film dynamics that eventually lead to chronic mechanical irritation and hyper-osmolarity.
Tear Film Deficiency typically leads to Damage of the Ocular Surface. This occurs via Sequences of Secondary Pathogenetic Factors in the tear film dynamics that eventually lead to chronic mechanical irritation and hyper-osmolarity.
The secondary alterations of the tear film lead to two main pathogenetic factors:
CHRONIC MECHANICAL IRRITATION
by increased Mechanical FRICTION due to wetting deficiency with ´dry spots´
HYPER-OSMOLARITY
spots of increased osmolarity
by increased evaporation of the aqueous phase due to a disturbance of the normal tear film structure
Increased mechanical friction and chronic mechanical surface irritation will always occur when the tear volume and thus the lubricative capacity decreases.
Hyper-Osmolarity is typically only associated when the loss in tear volume is due to increased evaporation of water from the tear fluid. This applies however, according to the present concepts, to the majority of dry eye patients because Meibomian Gland Dysfunction with a lipid deficiency and subsequent increased evaporation affects about 4 out of 5 patients as a primary cause.
Downstream EFFECTS of the main Secondary Pathogenic Factors (Mechanical Friction and Hyper-Osmolarity) are:
both of them lead to cell activation
with up-regulation of inflammatory mediators and
potential onset of inflammatory cascades.
Chronic negative influences decrease the cell viability and eventually lead to cell wounding and destruction.
TISSUE DAMAGE AND TEAR FILM DEFICIENCY ARE BOTH INTIMATELY INTERRELATED AND INTERDEPENDENT
Tear Film and and Ocular Surface Damage are closely interrelated and interdependent - in the normal physiology as well as in pathology. An intact tear film can only bind bind to an intact epithelial surface and the mucosal surface only remains intact when it is permanently kept moist by the tear fluid. In the "typical" Dry Eye Disease that the clinician sees in everyday practice Tear Film Deficiency is typically first and induces Surface Damage - whereas a primary Surface Damage is relatively rare although it may occur in certain conditions.
Thus, a typical downstream effect of Tear Film DEFICIENCY is the onset of Ocular SURFACE DAMAGE of the tissue. This shows how closely the tear film and the ocular surface are interacting and interrelated
In fact the tear film and the ocular surface tissue are interdependent because the moisture of the tears - that can only exist as a tear film in the exposed palpebral fissure - is the pre-requisite for the integrity of the moist mucosal tissue.
And, in return, only an intact mucosal epithelial surface can bind a pre-ocular tear film, which is the pre-requisite for visual acuity ... as explained in the Section for ´Ocular Surface´(for details please see there)
SURFACE DAMAGE CAN OCCUR PRIOR TO TEAR FILM DEFICIENCY – BUT THIS IS RARE IN TYPICAL DRY EYE DISEASE
A primary Ocular Surface Damage can occur in certain pathologies such as in Vitamin A deficiency. Sin such cases, which are however not what we consider as a "typical" Dry Eye Disease, the Tear Film Deficiency occurs later and secondary to the Surface Damamage.
Squamous Metaplasia is based on a changed epithelial differentiation into a different type of epithelium, with large flat cells and a loss of mucin-secretory goblet cell.
This leads to a mucin deficiency with decreased binding of the tear film to the tissue surface and can thus induces a Dry Eye Disease when it affects larger areas of the conjunctival surface in the palpebral fissure.
In "typical" Dry Eye Disease ... Tear Film Deficiency is first ... and Surface damage occurs downstream and later.
The "typical" Dry Eye Disease is defined by what the doctors see in their daily practice. Most studies on Dry Eye are performed in the reasonably well developed countries, where the individuals have a chance to see a doctor - and reverse.
In countries where a Vitamin A deficiency occurs due to insufficient diet - which tragically still affects many regions of our planet - this is not the case. Vitamin A deficiency inhibits the maturation of the ocular surface epithelium. This results in squamous metaplasia with goblet cell loss and mucin deficiency.
Such patients with dietary Vitamin A deficiency also suffer from Dry Eye Disease, but in these individuals, squamous metaplasia with a primary mucin deficiency constitutes a PRIMARY SURFACE DAMAGE - which is the most frequent underlying cause for Dry Eye Disease here. Tear FILM Deficiency come later in this case.
Other possible reasons for a primary Surface Damage
Other reasons for a primary Surface Damage with secondary Tear Film Deficiency can be e.g.:
a primary auto-immune disease such as e.g.
Sjögren´s Syndrome
Ocular Pemphigoid
other adverse immune reactions such as e.g.
Graft-versus-host Disease that may occur after bone marrow transplantation when the lymphoid cells of the graft attack the host tissue including the ocular surface
neural problems of any kind when the ocular surface tissue are deprived from the trophic function of innervation
or, e.g. accidents such as ocular burn that first destroy the surface tissue
... and several other possible reasons which have in common that they are all relatively rare compared to the ´ordinary´ Dry Eye Disease can can be seen everyday in the clinical practice as the most frequent disease type.
Therefore the typical ´downstream´ direction from Tear Film Deficiency to Surface Damage, as shown in the "Holistic Dynamic Concept for the Pathophysiology of Dry Eye Disease", practically holds true even though a primary Surface Damage is possible in Theory.
The Tear Film Deficiency and the Surface Damage are thus both addressed as ´Primary Pathology in the"Holistic Dynamic Concept for Dry Eye Disease" ... which may appear irritating at first glance.
TISSUE DAMAGE AND TEAR FILM DEFICIENCY ARE BOTH PRIMARY PATHOLOGIES ... AND ARE LINKED VIA VICIOUS CIRCLES
Vitamin A deficiency is one example that a primary Surface Damage is possible, other tropic problems e.g. due to pathology of the nervous system would induce similar effects. Such primary Surface Damage will than lead to secondary Tear Film Deficiency. But this is, altogether not the "typical" case in the more developed countries.
Since Surface Damage and Tear Film Deficiency are so closely interrelated, it appears justified and makes most sense from a more general patho-physiological perspective on Dry Eye Disease, when both intimately related pathologies of the Tear Film and Tissue are both designated as "Primary Pathology".
Chronic Inflammatory Pathways are a central component of OCULAR SURFACE DAMAGE
Chronic Inflammatory Pathways are a central component of the disease process of Dry Eye during Ocular Surface Tissue Damage. This is induced by the initial epithelial alterations due to tear film deficiency and may proceed into an immune-mediated mucosal inflammation, if it is not interrupted by therapeutic intervention, to a Degenerative Tissue Remodelling with Loss Of Function.
The initial Surface Tissue Damage that occurs in Dry Eye Disease by wounding and activation of the surface epithelium is the onset of a potential chronic inflammatory process - if this is not timely diagnosed and approached by suitable therapy.
Inflammation is initiated as a very basic protective and repair mechanism that applies tissue degrading enzymes and activates different tissue cells and the vascular endothelium to recruit further cells for help.
Thereby the inflammation tends to proceeds and become more severe,
from a clinical not visible SUB-Clinical Inflammation
into a CLINICAL Inflammation with the cardinal signs of inflammation such as redness, swelling and pain.
KEY EVENTS IN CHRONIC MUCOSAL INFLAMMATION
Some KEY EVENTS in chronic Ocular Surface Damage of Dry Eye Disease transform the primary protective Repair Mechanism of Sub-Clinical Inflammation into a clinically overt Destructive Chronic Mucosal Immune-Mediated Inflammation
During the chronic inflammatory activity due to the chronic presence of pathogenic stimulation in Dry Eye Disease with presence of tissue wounding and cell activation respective inflammatory mediators accumulate in the tissue with downstream negative effects:
the mucosal immune system can become deregulated and the process transforms into an immune mediated inflammation.
the natural physiological mucosal immune tolerance can be lost and thus
non-pathogenic and environmental antigens but also own tissue antigens can be presented to the resident cells of physiological protective Eye-Associated Lymphoid Tissue (EALT)
with the risk of auto-immune disease.
During the ongoing chronic rounds of inflammation the tissue repair attempts become frustrane and end up in a Degenerative Tissue Remodeling with formation of new blood and lymph vessels with degradation of the collagen matrix and reparative scarring.
VICIOUS CIRCLES typically occur in Dry Eye Disease and give rise to a self-enforcement and worsening of the disease process
Vicious circles are pathogenetic effects, i.e. negative effects promoting the pathology, that act BACK onto themselves and therefore reinforce the disease process.
Often this occurs via the action of interposed further pathogenetic factors and is therefore not always immediately evident at first glance. Vicious circles are not necessarily dependent on inflammation even though an inflammatory process typically gives rise to vicious circles.
As an example, Tear Film Deficiency and Surface Tissue Damage are linked via a Vicious Circle that does not necessarily depend on inflammation. In this pathological reinforcement loop Tear Film Deficiency causes Surface Damage and a damaged Surface is causing more Tear Film Deficiency which will then make the Surface Damage more severe ... and in return.
Such a vicious circle typically goes on and on with progressive worsening of disease until it is eventually recognized and interrupted by a suitable intervention that depends on the nature of the involved factors.
In the Vicious Circle that connects Tear Film Deficiency and Tissue Damage an INTERRUPTION is often possible e.g. simply though the application of suitable tear supplementation in order to decrease friction and normalize a hyper-osmolarity if this exists.
A tear supplementation is however only "suitable" and thus effective when it is patho-physiologically adequate - this means, when it indeed contains the factors that are actually missing.
In the most frequent case of a primary lipid deficiency the tear supplementation should contain lipids and specifically of that type, or, if it exists, another substance with the same action, that is needed to reform a superficial lipid film for retardation of the aqueous hyper-evaporation.
More Severe Vicious Circles and Disease Dynamic occur INSIDE the TISSUE in SURFACE Disease
The Surface Tissue Damage that occurs in Dry Eye Disease and proceeds via a sequence of secondary pathogenic factors - with chronic mucosal inflammation as a major amplifying factor.
The disease process starts with wounding and activation of the epithelial surface cells. This leads to their activation with the intention to mount a protective and reparative answer in form of a sub-clinical inflammation in order to cope with the wounding.
When the irritation and wounding of the tissue becomes chronic, however, the subclinicalreparative answer the subclinicalinflammation amplifies into a more severe clinicallyvisible inflammation.
This can lead through the chronic inflammatory micro-milieu to a de-regulation of the mucosal immune system and thus transforms into an immune-mediated chronic mucosal inflammation with the risk of progressing into an auto-immune disease - as experimentally shown.
Degenerative tissue remodeling with loss of function is a possible end Stage
The possible end stage of severe chronic inflammatory Dry Eye Disease when occurring self perpetuating vicious circles can not be interrupted sufficiently ... can be a degenerative tissue remodeling with loss of function.
Downstream mighty Vicious Circles originate from abnormal cell differentiation in the tissue with angiogenesis and are driven by the chronic inflammation that gives rise to the corrupted tissue differentiation. Squamous metaplasia with loss of goblet cells and mucins is also, at least in part, promoted by inflammatory mediators.
The Surface Tissue Damage that occurs in Dry Eye Disease and proceeds via a sequence of secondary pathogenic factors - with chronic mucosal inflammation as a major amplifying factor - also involves the tissue of the ocular GLANDS. This leads to pathological carousels of Gland Dysregulation.
These are large vicious circles that connect the disease process in the surface of the conjunctiva and cornea with disease processes inside the glands and can lead to degenerative tissue remodeling of the whole ocular surface with loss of function.