Deeper Insight into … CONTACT LENSES
… Types, History, Schedules, Materials & Fitting … and of course the Ideal Contact Lens
Topics
A short history of Contact Lenses
A short overview of Contact Lens TYPES and their HISTORY.
Contact lenses that were not restricted to mere phantasy but could actually be worn – however without much ´comfort´ – are around now for roughly one and a half centuries. Contact lenses were greatly improved during about the last 50 years, primarily due to the advent of new materials and other technological advancements.
The first contact lenses were scleral lenses made from glass
In the last quarter of the nineteenth century different people in Europe have worked on making a real contact lens, that is practically wearable.
This is associated with names like FICK, MÜLLER, KALT, GIRARD and probably others. Due to the restriction to ´natural´ materials, these lenses were made from glass blown spheres.
The spheres were later cut into a size with a diameter larger than the cornea because the cornea is very sensitive and it was immediately clear, that a contact lens would not be tolerated on the cornea. Therefore it had to rest on the surrounding scleral wall of the eye ball. Such contact lenses were thus termed “Scleral Contact Lenses”. This name is valid until today … even though the Sclera is covered at the anterior side, i.e. at what is termed the ´Ocular Surface´, by the thin and almost translucent organ of the Conjunctiva. Scleral contact lenses thus practically rest on the conjunctiva of the eyeball, the bulbar conjunctiva, and not on the sclera..
These historic scleral contact lenses could only be worn for some few hours a day, and even then, it could be necessary to anesthetize the ocular surface by (topical) cocaine. But still, in principle a ´wearable´ contact lens was born by then.
Rigid lenses from PMMA polymer were the first artificial/´plastic´ lenses
In the end of the 1920s a new “artificial glass” material was developed. It is a polymer termed ´PolyMethyl MethAcrylate´ (PMMA). It is also known as ´Acrylic Glass´ or more often known under the brand name ´Plexiglas´. From the 1930s on, the first ´plastic´ lenses were manufactured from PMMA and slowly went into broader usage. In Germany the, then young, Contact Lens Pioneer Heinrich Wöhlk from Kiel, started experimental work on Contact Lenses from Plexiglas and in 1940 he produced the first fully ´plastic´ contact lens. As a dedicated inventor he tried the lens on his own eyes. As he had a severe hyperopia, and found that this new PMMA material had a superior wearing comfort compared to the previous glass blown and cut lenses.
1946 Heinrich Wöhlk started his company that manufactured the first Rigid Plastic Contact Lenses at home in a garage style environment – very much like about 30 years later the personal computer pioneers started with their foundations. Wöhlk is still a leader in Contact Lens Technology and manages to hold the full range of material supply and manufacturing in-house.
The term ´plastic´ may be misleading to some extend, because the plasticity of these lenses was quite limited and they were similarly hard as glass-lenses. They share with glass also the disadvantage that PMMA is completely impermeable for oxygen. Therefore the cornea can only get enough oxygen and nutrients when the lenses are sufficiently movable to allow continuous tear exchange under the contact lens and when the wearing time is restricted during daytime ... at most.
Hypoxia of the cornea in contact lens wear can typically lead to neovascularization of the corneal margin vessels
Hypoxia of the corneal tissue underneath the contact lens leads to typical changes. Most obvious and well-known is probably the progressed growth of the vessels of the marginal limbal arcade. Normally the vessels stop at the beginning of the cornea but when the cornea becomes hypoxic, i.e. has a lack of oxygen, the vessels grow onto the cornea to bring oxygen closer to the center. This is termed as ´Neovascularization´. (please see the image).
Since PMMA contact lenses require a long adaptation period, a wearer of PMMA rigid corneal lenses must be really determined to use them
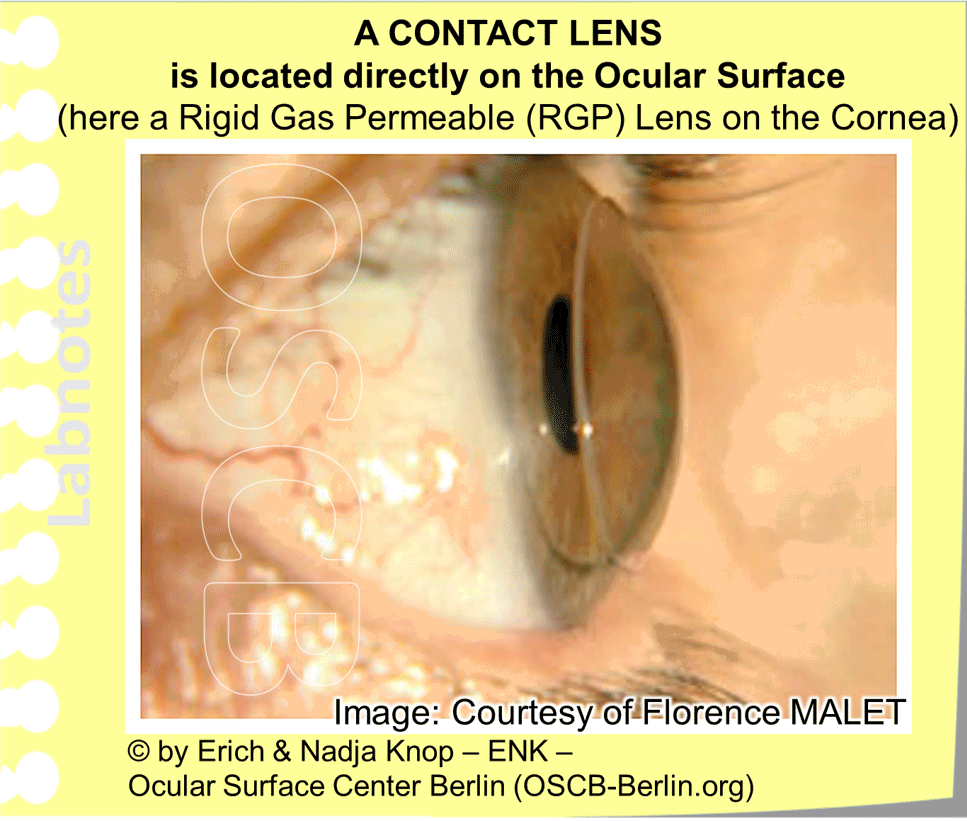
Today Rigid Gas Permeable (RGP) Contact Lenses are available ... but often receive less attention than they would deserve
In the 1980s stiff, e.g. rigid, materials with a very good oxygen permeability were developed. These lenses were thus termed ´Rigid Gas Permeable´ (RGP) contact lenses.
RGP contact lenses have a superior inert material quality, clarity and durability together with a high oxygen transmission
This seems to make up ideal characteristics … but they are still rigid – This means that a certain ´adaptation period´ of typically some or more days is necessary before they are tolerated without discomfort.
Rigid Gas Permeable lenses are definitely much better tolerable than the previous PMMA lenses. Therefore an individual must be only be somewhat determined to use this excellent lens type - which is still not too often the case compared to ´soft´lenses.
However in many cases a rigid material is preferable or even distinctly necessary, i.e.
for ´ironing out´ a moderate astigmatism or
for fitting toric lenses for high astigmatism that have different diopters in different axes, or
for ´bifocals´ or ´progressive contacts´ that are useful in presbyopia, and act similar to respective spectacles,
Then, RGP contact lenses are certainly the lens of choice. This applies also for fitting a contact lens in a patient with a protrusion of the cornea, termed keratoconus.
Soft hydrogels brought the opening of the mass-market for contact lenses
Contact lens materials that are less rigid, and thus more ´soft´, were developed in the 1960s by two Chech chemists (Wichterle and Limm) by the introduction of water into the polymer of the lens material - which was still typically based on PMMA.
The water in the polymer-material allowed for the oxygen transmission and also for the softness of the lens. Therefore oxygen transmission and flexibility were the greater the higher the water content of the lenses reached.
Well remembered, at least in Germany, are e.g. Soft Contact Lens Types such as ´Weflex 55´ and ´Geaflex 70´ from the end of the 1980s, where the number indicated the water content in percent. The water content in return pointed to the oxygen permeability, softness and potential duration of continuous wearing hours that could be expected. from the lens. These contact lenses from the famous smaller manufacturer Wöhlk, in the city of Kiel, were candidates for the first contact lens studies where members of the OSCB were involved. Both of these lenses set standards of excellent construction and wearability and they are still produced today.
SILICONE – the miracle molecule – allows high oxygen permeability without water
Because of the limited oxygen permeability of conventional hydrogels further research led in the 1990s to the introduction of SILICONE-Hydrogels into the mass market of soft contact lenses. Silicone has the great advantage that it has a very high oxygen permeability, higher than water itself. Silicone Contact Lenses thus improved or abolished alterations of the ocular surface due to lens-related hypoxia, such as progression of the marginal corneal (limbal) arcade vessels, onto the cornea.
Due to the very high oxygen permeability of silicone, the effective oxygen permeability in respective silicone hydrogel lenses is at least 10 times higher than in conventional hydrogels that were available at the time of silicone introduction. Silicone was thus the ´missing link´ for contact lenses to allow full ´extended wear´, i.e. overnight or even for many days without hypoxia of the cornea.
Pure Silicone is almost non-wettable – which made some material improvements necessary
On the other hand, silicone has a natural poor wettability by aqueous solutions.
This is conceivably the reason why silicone is typically used in wet bathroom environments to seal the space all around equipments such as bathtubs against water entry into the surrounding walls ...
Poor wettability may not appear as an immediately ideal characteristic for a contact lens that is swimming in the tear film. ... all day long ... and at night if necessary.
During the evolution of Silicone based contact lens materials over the last two decades, many advancements of material properties have been introduced.
Such material modifications of the silicone-hydrogels can be made either by introducing other materials into the polymer or by modifying the surface of the contact lens - the silicone-hydrogel contact lenses were thus technically ´convinced´ to acquire sufficient wettability. together with lower modulus, i.e. higher flexibility and softness. (please see below)
An example for material improvements of silicone hydrogels is the ´water-gradient-technology´ by ALCON Inc.. This technique provides a contact lens with a silicone core for the basic contact lens properties which gradually transforms to the surface into a polymer with a higher water content. It is proposed that parts of the polymer molecules at the lens surface are even able to form something like a functional equivalent to the water-binding glycocalyx molecules of the ocular surface cells.
Silicone lenses have a higher ´MODULUS´ – they are more stiff than ordinary Hydrogel Contact Lenses
Silicone has another important material characteristic that has lead to increased popularity of the term ´MODULUS´.. Modulus refers to the ´Stiffness´ of the lens material. Modulus is not exactly the same as ´Rigidity´ i.e. even though a silicone-hydrogel contact lens has a higher modulus it does not become as ´rigid´ lens as an RGP lens. But the effect of a higher modulus at least results in a lower flexibility of the lens on the eye and thus of higher mechanic interaction with the ocular surface tissues. Therefore the first silicone lenses could require a certain short adaptation time.
Generally, very thin Silicone Contact Lenses with an increased ´natural´ stiffness (modulus) have an increased risk for causing epithelial slits (SEALs). The risk is however only a few per cent of the users of such lenses and epithelial splits can also occasionally occur in conventional hydrogels without silicone. The risk for epithelial splits is therefore probably also related to the very thin lens design that may, even with a optimized geometry of the lens margin pose a higher risk to ´cut´ into the epithelium.
Which is the best Soft Contact Lens ?
Silicone lenses became the nowadays (almost) first choice not only for soft contact lenses but also for contact lenses in general. Silicone also offered the first really suitable contact lenses for EXTENDED WEAR - which refers to overnight wear - without too much risk of corneal anoxia and respective damage. However, also the ´conventional´ hydrogel contact lenses without silicone have seen a lot of refinements in material and lens geometry, so that the question for the ´BEST´ Soft Hydrogel Lens is not easy to answer.
Different Basic Types of Contact Lenses
For most contact lens wearers the choice of lenses comes basically down to 2 types
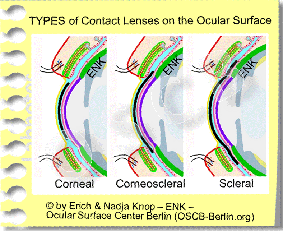
Different TYPES of Contact Lenses on the Ocular Surface - Contact lenses are used in different types that have a different diameter and thus cover different parts of the ocular surface.
The wearing experience with a contact lens most influenced by two parameters of Contact Lenses.
SIZE – of the lens, i.e. how large is it on the eye and
MATERIAL – i.e. is it ´hard´ or ´soft´
These parameters are typically linked, therefore the effective range of basic contact lens TYPES is relatively easy to overview ... if specialty lenses are excluded.
In fact, for most users, the variety of contact lenses basically comes down to two types that differ in their ´comfort´ - which typically does not refer to long term satisfaction and tissue compatibility, but to the fact whether or not the contact lens is initially distinctly felt as a foreign body on the eye and thus needs a certain adaptation time ... or not. So, the typical contact lens wearer just distinguishes between ´HARD´ (i.e. rigid and small) and ´SOFT´(i.e. hydrogel and corneo-scleral) Contact Lenses ... and everything else goes without saying.
If we integrate the large scleral lenses, for historical reasons and because they have developed into a high-tech and versatile medical tool for several kinds of chronic ocular surface conditions it would make sense to have a view at at least THREE TYPES of Contact Lenses:
Scleral Contact Lenses – ´The Tall´
Historically, the first contact lenses were very large in order to vault over the cornea and rest on the sclera. These lenses were stiff, because in the old days nothing soft was available, and they have continued to be manufactures as stiff or rigid lenses because this is necessary to produce the vault.
More recently many high-tech advancements were achieved for scleral lenses that allowed many improvements in fitting and wearing. ´Sclerals´ offer promising medical advancements in many medical indications as will be discussed in more detail below.
Corneal Contact Lenses – ´The Rigid´
Small contact lenses with a diameter smaller than the cornea are the other extreme ... compared to scleral lenses. The material properties have changed from glass over PMMA-plastic to nowadays highly oxygen permeable polymers. They are now the basis for the standard type of small rigid gas permeable (RGP) contact lenses. The characteristics of ´small´ and ´rigid´ typically address these small corneal contact lenses.
Corneoscleral Contact Lenses – ´The Soft´
´Intermediate´ size refers to a size larger than the cornea but not so far onto the bulbar conjunctiva as the large sclerals reach. These lenses are termed corneo-scleral lenses and they typically reach onto or just beyond the corneal limbus. This was the ´final´ step in contact lens development when soft hydrogels became available. These lenses nowadays have the widest distribution with over 90% market share. So eventually SOFT & CORNEO-SCLERAL is another and the most frequent combination of contact lens characteristics of size and material.
WEARING SCHEDULES
Wearing Schedules
Contact lenses are typically worn during daytime activity when visual acuity is important and they are thus taken out overnight when the eye is closed and vision is no longer relevant. Therefore daytime wear is the standard wearing schedule and overnight wear is termed as ´extended´ wear.
Daytime Wear
This wearing schedule with limited daytime wearing hours was historically dictated by ocular surface sensitivity because the glas contact lenses very uncomfortable and could hardly be worn longer than some few hours. The later plexiglas (PMMA polymer) materials and particularly soft hydrogel lenses were were much more comfortable to wear but then the metabolic factors in terms of oxygen supply became relevant for limitation of wearing time. Plexiglas is completely impermeable to oxygen which became better when water was introduced in the newly developed hydrogel materials but the oxygen supply was still too limited for more than daytime wear. Even then too long wearing hours or heroic customs to perform ´extended wear´ with ordinary hydrogels typically resulted in corneal hypoxia with neovascularization of the limbal vascular arcades.
Extended Wear
Extended Wear refers to the continuous wear of a contact lens during 24 hours including sleep with closed eyes.
Some of these extended wear lenses can even be worn for several days in a row, up to one month - This is sometimes called ´CONTINUOUS WEAR´.
Extended wear became possible only with the advent of the extremely oxygen permeable silicone hydrogels in the end 1990s.
Replacement Schedules & Disposables
Simplified manufacturing methods and mass production have allowed it to offer Disposable Contact Lenses at affordable prices. Disposable contact lenses, nowadays at best daily disposable lenses, are thrown away after wearing them … and the next time when the user decides to wear a contact lens, i.e. probably next morning, a completely new and clean lens is used.
The term disposable is not completely new
The term disposable is not completely new, because basically contact lens have always been disposed after a certain time. The term of a ´disposable contact lens´ only applies to soft hydrogel materials because ´rigid gas permeable´ contact lenses have an excellent material stability and typically do not age that much as soft hydrogels.
´Ordinary´ (soft hydrogel) contact lenses in former times were disposed when they had accumulated too many alterations and damage over time
due to aging processes of the material itself, with loss of water content, increasing degrees of stiffness, fissures and splits or other destructions of the contact lens margin
due to the accumulation of depositions on the lens - typically with materials from the Tear Film such as proteins or lipids or jelly bumps. Depositions can, apart from building up on the surface of the lens, also alter the material of the lens and introduce holes as can occur in jelly bumps. Bacterial contamination with biofilms are difficult to clean away and must also be considered as ´deposits´, apart from their potentially infectious nature.
The difference in explicit ´Disposable Lenses´ mainly is, that these are regularly disposed based on a fixed schedule independent of actual ageing or alterations. In fact, the basic idea is, that these contact lenses are replaced before ageing and with loss of some main quality characteristics.
There are contact lenses with different material properties and prices for different replacement schedules
There are contact lenses with different material properties and prices for different wearing schedules i.e. ´Day´ , ´week´, ´month´ and ´year´ contact lenses. This nomenclature indicates, after which time periode the lenses have to be replaced.
The easiest case is a daily lens, because there a new contact lens is inserted every morning.
The ´year´ lenses basically refer to ordinary soft hydrogel lenses because a hydrogel contact lens had always typically seen its best times after a time of about one year and needed to be replaced by then
Week, 14 day and month lenses have an intermediate replacement date.
Generally a contact lens can be made the thinner and thus often more comfortable to wear the shorter the wearing schedule is.
The replacement schedules for disposable lenses do not necessarily include ´Extended Wear´ overnight Capability
However, these ´ordinary´ wearing schedules do not necessarily include ´extended wear´ characteristics, i.e. the option to wear the contact lens overnight - not even in the ´daily´ lenses. This is because the oxygen supply is strongly decreased by the closure of the eyelids overnight.
Therefore, in every Replacement Schedule that is longer than 1 day, the contact lenses still have to be cleaned and then stored overnight in a container. This leaves the principal risk of problems with deposits, hygiene and bugs ... but all these issues are reduced - the more the shorter the replacement schedule is.
An extended wear schedule requires a contact lens with a very high oxygen permeability. This is typically only available in silicone-hydrogel contact lenses, which tended to be higher-priced than ordinary hydrogel lenses. Meanwhile there are also Disposable Silicon-Hydrogel Contact Lenses available - a contact lens type that is disposable and highly oxygen permeable and thus suitable for extended wear of apparently even up to 30 days. The first disposable silicone hydrogel is the ´True Eyes´ from Johnson and Johnson.
Disposable Contact Lenses … make all the Hygiene so much easier
A daily disposable is the best hygienic option to avoid infections
Thereby Disposable Contact Lenses or lenses for longer replacement schedules but with continuous wear and thus without clearing and storage improve some important issues of Contact Lens hygiene.
From the aspect of HYGIENE, a daily disposable contact lens that does not need cleaning and storage after wear is certainly the best option.
Frequently changed Disposables also reduce the Risk for Contact Lens Associated Papillary Conjunctivitis
Disposable Lenses do not only reduce infectious contaminations but also LENS DEPOSITS of tear film components. Such depositions can act negative in different ways:
they represent a mechanical stumbling block and that increases mechanical friction of the lens onto the tissue
the deposited materials, even though they derive primarily from the own tear film, often induce a hypersensitive allergic response because the material is denatured and thus different from the normal structure. Chronic mechanic and antigenic irritation of the tarsal conjunctiva can typically lead to a condition termed ´Giant Papillary Conjunctivitis (GPC), that was originally discovered and described by Donald KORB from Boston, in Contact Lens Wearers. GPC can however also occur due to other stimuli of foreign material, such as sutures that are exposed at the surface or a keratoprosthesis. A newer term that describes specifically Contact Lens Associated Papillary Conjunctivitis is abbreviated as CLPC or CLAPC. As a difference to conventional Ocular Allergy, this contact lens associated form is not related to or based on an Immunoglobulin E (IgE) mediated allergic process.
Apparently other, previously unknown complications, may now occur in Disposable Lenses
It must not be forgotten that a used disposable contact lens must in fact be removed and disposed before applying a new one ...
This may seem of no relevance but recently there was a report in the British Medical Journal about a patient who was seen in the eye clinic for cataract surgery. This happened to be an experienced contact lens wearer who had used contact lenses for decades.
During closer investigation of the eye before surgery, a peculiar mass was uncovered from the inscrutable depth of the conjunctival sac.
It turned out to be an accumulation of dozens of disposable contact lenses, that had become stacked one over the other (please see the image). After more careful further investigation, altogether 27 retained disposable contact lenses were uncovered from the conjunctival sac.
Surprisingly all these retained lenses had not caused any major discomfort to the patient - which may probably give some indication, how far a contact lens adaptation process can reach.
We may hope that this is an isolated case ... but ... when you are nex time looking for your contact lens you may consider to have a look into the eye.
WHICH is the IDEAL Contact Lens ?
Which is the ideal Contact Lens? Which Contact Lens should I chose? Which is the right contact lens for me?
The choice of Contact Lenses for most wearers basically ends up with two types of Soft Lenses – Conventional Hydrogels and Silicone Hydrogels
The question about the BEST Contact Lens would put a potential judge similarly in trouble as it once happened to the poor shepherd PARIS, who was the son of the legendary king of the legendary city of Troy. He was asked to chose for the most beautiful one among the three Greek goddesses HERA, ATHENA and APHRODITE ... of whom one was more beautiful and tempting then the other ... not to tell about the potential anger of those who would have to be rejected ........ The fact that he had to inspect them nude is probably evidence, that he may have been an early morphologist. We don´t tell here what Paris did but stick to contact lenses, which is probably safer.
In order to make the situation even more delicate, each of the goddesses promised Paris a tempting reward in order to convince him to vote for her. In case of contact lenses, Hydrogelia would probably promise ´eternal wettablia´, Siliconia would likely promise ´total oxyphilia´ whereas Rigidia would probably promise ´eternal inert stabilia´ ........ hmmmmm, how about that ?
Two lines of evidence presently make most contact lens wearers end up with one of two types of potentially appropriate contact lenses.
One line of evidence is the fact that the Rigid Gas Permeable (RGP) contact lenses have many superior material properties … BUT … they are ´rigid´ and thus require a certain adaptation period of some or more days.
This makes them uninteresting for most potential wearers who just want to wear a contact lens with immediate and full comfort and satisfaction without any further considerations.
Immediate comfort appears more important for most contact lens wearers than a potential long term tissue compliance of the contact lens with the ocular surface tissue that can only be judged in the long run and by an experienced clinician based on ´hard data´.
Therefore personal preferences, i.e. mostly comfort, are important and bring us closer to the answer of the initial question of ´WHICH is the BEST Contact Lens´
The other line of evidence is the great evolution of soft contact lens materials including of the highly oxygen permeable but initially rather stiff and poorly wettable silicone. This has lead to a great improvement of CONVENTIONAL Hydrogels as well as of SILICONE Hydrogels, that still have superior oxygen permeability.
The two types of SOFT contact lenses are relatively similar but still have some slight differences in material and thus in characteristics, properties, pros and cons, and eventually indications for use.
Which is the ideal (soft) Contact Lens
When we have cut down question of the ´BEST Contact Lens´ by comfort to the best ´SOFT´ contact lens, then another issue becomes important and this is: ´PURPOSE´ – i.e. what do I need the contact lens for? or ... which Contact Lens characteristics do I need for my type of wear ?
A SILICONE contact lens is certainly of advantage when Oxygen is the main issue. This is the case when either a very long wearing time is intended, such as extended wear, probably for many days in a row - which is possible - some lenses are proposed for up to 30 full days and nights. The other case is that a prospective wearer has already worn contact lenses over a longer time and already has signs of corneal hypoxia, such as progressed growth (´neovacularization´) of the peripheral marginal arcade vessels at the limbus. Since the growth of these vessel cannot be reversed and further growth may impair the corneal transparency, the use of contact lenses is then typically suggested to be discontinued ... or potentially silicone lenses could be tried as a ´last choice´ with frequent follow up controls.
Many other things can be of importance i.e. the volume of tears in patients with Dry Eye Disease which requires a highly wettable lens.
The composition of the tears can play a role. If there is a high content of proteins or lipids (normal or altered in MGD) a lens should be chosen that does not tend to pick up this material. In Dry Eye Disease there are also often increased amount of cell debris from the continuous micro-trauma of the surface within the tear film. Depending on IF and WHICH deposits occur (lipid or protein) the lens type can be chosen to decrease the rate of deposition of that particular substance.
The principally higher modulus, i.e. stiffness of Silicone lenses is grossly ameliorated by improved material technologies. If the issue really is optimal Oxygen permeability, then a slightly increased stiffness does not represent any major problem.
What is the best quality contact lens – Immediate comfort vs. longterm tissue compatibility
The question for the ´best´ Contact Lens is almost impossible to answer because there is a multitude of potential criteria. Therefore it makes some sense to narrow it down by integrating ´for the eye´. to ask ´Which is the best Contact Lens for Ocular Health and Integrity´. This is still difficult to answer.
There are probably at least to important criteria that are, however, somewhat different:
Immediate comfort
The appreciation of a wearer for a contact lens is typically driven by the immediate comfort. It is not difficult to guess this from the overwhelming market share of soft contact lenses that basically do not require any adaptation time to get used to a contact lens on the eye. - ´ If I don't ´feel it it must be a good lens ! ´
Longterm tissue compatibility
The other issue that comes closer to the topic of ´best for the eye´ refers to something distinctly different which is the influence of the lens on the tissue health and integrity. - This ends up as : ` What we need is hart clinical data from many follow ups´
Who is judging what ?
Whereas the wearing comfort can only be decided by the wearer himself, the influence on the tissue can typically better or only be answered by a clinician on the basis of ´hard´ clinical evidence from respective tests and signs. Also, a qualified judgement on the tissue compatibility can often better be answered after a longer wearing time and by overview of a larger patient cohort.
The reason is, that some signs of tissue alteration such as e.g. ´epithelial splits´ (a specific type of erosions) may occur immediately or early but even then a larger patient cohort is necessary because the may only occur in a small number of patients. Other indications of a negative contact lens impact on the tissue such as e.g. signs of corneal hypoxia in the form of limbal blood vessel neovascularization or decompensation of the corneal endothelium typically take a longer time in the range of years, even though they are potentially severe and should not be overlooked.
Some Considerations for Contact Lens Fitting
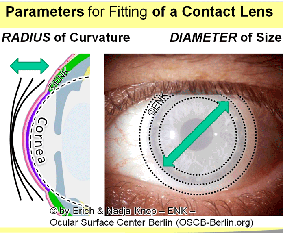
A Contact Lens must be fitted to the radius of curvature and to the size-diameter of the cornea … to swim freely in the Tear Film
In order to swim freely within the pre-ocular tear film a contact lens has to be fitted as closely as possible to the shape of the underlying tissue - which is in most cases the cornea. Such fitting is the prerequisite, that the lens can be worn with minimal mechanical interference (in terms of pressure and friction) on the ocular surface.
The two main technical parameters for fitting a contact lens are
Radius of Curvature of the Cornea that has to be translated into the ´base curve´ of the contact lens
Size diameter of the lens that depends on the type of contact lens and the intended wearing characteristics.
Both, the Diameter as well as the Radius, distinctly influence the fit of a contact lens on the eye. This relates to a loose or tight fit, to the amount of movement during the blink that influences the tear exchange under the lens, and to the (unwanted) potential mechanical interaction of the lens with the tissue.
Typically it is aimed to achieve a parallel fit where the shape of the contact lens approximates that of the underlying tissue as closely as possible, so that the lens has everywhere the same distance to the tissue. The weight of the lens and the resulting pressure is then most equally distributed across the surface of the contact lens. Depending on the actual contact lens type and the applied fitting principle some changes to this ´rule of thumb´ are possible.
The less flexible and the larger a Contact Lens is, the more exact the fitting must be
The less flexible and the larger a Contact Lens is , the more exact the fitting must be - This must however not be translated into the reverse conclusion, that a very flexible lens or probably all ´soft´ contact lenses do not need appropriate fitting. This is not very advisable.
Since every eye is different and every contact lens basically always is a ´foreign body´ on the ocular surface, there is no ´one fits for all´ in contact lenses and every contact lens must be fitted as precisely as possible.
When the base curve/ RADIUS of the contact lens is too different from the curvature of the cornea on which it sits this will distinctly influence the fit of the lens on the eye. Typically the fit and movement of the contact lens is impaired, and such a lens, in return, can exert negative influences on the ocular surface.
When the contact lens is radius too steep compared to the cornea, it will sit too tight and does not move sufficiently. The periphery of the lens, i.e. the contact lens margin, exerts too much pressure on the eye and can leave imprinting marks in the epithelium, that can be seen when the lens is removed or when it is slightly move by a finger.
When the contact lens radius is too flat, it will sit very loose and is unstable. Such a lens will typically rest just with its middle part on the cornea and thus exerts pressure on the corneal center.
The size of DIAMETER of the contact lens also has influence on the fit,
The size of DIAMETER of the contact lens also has a certain influence on the fit of the contact lens even when the base curve remains the same. A larger lens (with the same base curve) tend to fit tighter and move less, whereas a smaller contact lens (with the same base curve) tends to fit more loosely and moves more.
Fluorescein vital stain can be of great help for contact lens fitting
In contact lenses that tolerate the application of fluorescein vital stain without taking it permanently up (which is unluckily not possible in many soft lenses), the tear film behind the contact lens can be nicely stained. It can be directly seen how intensely stained, i.e. deep, the retro-lental tear layer is – which translates into the distance from the tissue. A parallel fit would shows a homogeneously stained retro-lental color and thus tear film thickness. Depending on the actual lens design and the intended fitting strategy, there can be some modifications for optimal contact lens fit.
Some general considerations about the ocular surface condition and tears are certainly also necessary for fitting
As mentioned earlier, it is of course important to take note of the ocular surface situation and tear film parameters – This includes the: Diagnostic Techniques that are used for the Evaluation of Dry Eye Disease:
TEAR FILM
tear volume, often measured easiest by estimating the tear meniscus height
viscosity of the tear film
cell detritus in the tear film
experience with deposition of materials on previous contact lenses
etc ...
TISSUE
evidence of pre-existing signs of hypoxia, e.g. neovascularization of the limbal vascular net
evidence of pre-existing signs of epithelial microtrauma as seen by vital staining
at the bulbar surface
at the posterior lid margin (as Lid Wiper Epitheliopathy, LWE)
corneal irregularities
etc ...
PURPOSE and WEARING SCHEDULE
time of daily wear
possibly extended wear
disposable lenses
etc ...
OPTICS
higher diopters that may require thicker lens materials
higher astigmatism
etc ...