DEEPER INSIGHT into ...
The FUNCTIONAL UNIT – Regulatory Systems
The anatomical unit of the ocular surface is joined by regulatory systems into a functional unit
Members of the Ocular Surface Center Berlin have devoted their scientific energy to the concept of an Ocular Surface Anatomical and Functional Unit for about 3 decades.
Nowadays this is a cornerstone in the conceptual understanding of health and disease at the ocular surface.
The First Publication in the international scientific literature database NLM PubMed that concerns the Concept of an Ocular Surface Functional Unit and that has the words „Functional Unit“ and „Ocular Surface“ in the Title was actually published in 2000 at the Maui Congress of the Tear Film and Ocular Surface Society (TFOS) - which is the major meeting in the field - and was later published in the respective book article 2002 by Members of the OSCB.
... this was also one of the last meetings where we, and probably many other colleagues, had used ´glass slides´... does anybody remember these times ??? ;-)
The organs of the Ocular Surface are joined by a coordinated action of the same regulatory systems:
REGULATORY SYSTEMS are of major influence of the differentiation and function of the Ocular Surface Organs.
The Nervous System
The Endocrine Hormonal System
The Mucosal Immune System
When the regulatory systems fail ... this leads to onset of basic underlying factors for ocular surface disease
Basic underlying factors for Ocular Surface Disease lead to the prototypic form – which is a disturbance of wetting and film formation ...
... it is for obvious reasons termed as ´Dry Eye Disease´
because there is a lack of / deficiency in the secretion of the tear film components and/ or the eye lid function:
Tear film component deficiency
Lipid Deficiency
Aqueous tear Deficiency
Mucin Defiency
Lid function deficiency
Eye Lid and Blinking Deficiency (LBD)
The REGULATORY SYSTEMS of the Ocular Surface
The regulatory systems provide the Ocular Surface organs with signals for the growth, maturation and functional regulation of the anatomical organs.
Some of the signals are of physical nature such as hormones and the soluble factors and cells of the mucosal immune system
other factors are immaterial (in the widest sense) such as the electrical signals of the nervous system.
As we will see, the brain is not only important for many aspects of life in general - but it also determines the action of the regulatory systems:
obviously ... the nervous system, and
(less obvious) it is the ´CEO´ of the endocrine system ... and, when we think of psycho-neuro-immunology ...
the brain also influences the immune system.
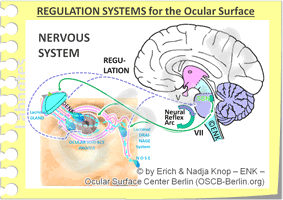
The NERVOUS SYSTEM is connected via afferent nerves (here interrupted blue lines) from the Ocular Surface and efferent fibers (here solid green lines) to the Peripheral Organs. Both fiber types have their center in the regulatory un, it of the Brain Stem of the Central Nervous System. The Nervous System performs the REGULATION of the tissue function in a neural reflex arcs via the cranial nerves V (trigeminal) and VII (facial) ... but is certainly also concerned with the Perception of Neural Sensations and of Feelings of PAIN ( - please see further down here).
The nervous system is probably the first system about which extensive research and concrete evidence for its relevance for Ocular Surface Function existed.
Clinical evidence for a lack of blinking and eye closure in facial nerve palsy or on the lack of extensive secretion in peripheral nerve damage is well established.
The nervous system is necessary to initiate and regulate the Eye BLINK - and the BLINK is necessary to transform the tear fluid into the essential tear film. The blink must occur frequent enough to be quicker than the limited stability of the film and must be full, which refers to full closure of the eyelids before they open again. So, in a way, the Tear Film is slave to the rhythm of the blink
The innervation of the eye occurs by the cranial nerves. They connect via afferent fibers from the Ocular Surface and efferent fibers to the Peripheral Organs the central regulatory unit of the Brain Stem to the Ocular Surface.
The cranial nerves encompass, apart from the somatic sensory and motor nerves, also autonomic fibers of the sympathetic and parasympathetic systems. The parasympathetic system is of prime importance for the secretion of glands.
The posterior lid margin is almost as sensitive as the central cornea ... due to the High density of Nerve fibers
The region with the highest density of sensory nerve fibers is the cornea but the posterior lid margin in the region of the Lid Wiper follows with similarly high nerve fiber density and thus sensitivity. This explains e.g. that the adaptation phase to a contact lens on the eye does does not only depend on an irritation of the cornea but also on alteration of the posterior lid margin, where it can lead to Lid Wiper Epitheliopathy (LWE).
The lid margin alteration termed as LWE was also found as one major route to explain Contact Lens Discomfort (CLD) as reported 2013 in the International workshop report on CLD of the ´Tear Film and Ocular Surface Society´ (TFOS, www.tearfilm.org - can be downloaded from their homepage).
Regulation of functions at the Ocular Surface
The ocular surface organs are linked to neural reflex arc via the afferent sensory cranial nerve V (trigeminal) and via the efferent motor fibers of the cranial nerve VII (facial). The reflex arcs typically link peripheral sensors at the ocular surface, which are either special receptors or simply free nerve endings, via the regulatory center of the brain stem, to efferent structures. Efferent structures can ´respond´ a suitable answer that changes the information of the sensors - typically by improving an unsuitable situation in the periphery – back to the normal expected input.
The ocular surface organs are connected via nerves to the brain stem. Neural Reflex Arcs between sensory nerves (typically trigeminal) and motor nerves (typically facial) regulate functions such as tear secretion or blinking. Here, blinking is triggered by a break-up of the tear film that leads to irritation of corneal sensory nerves.
A stimulus such as an irritation of epithelial cells and eventually of nerve fibers, by e.g. dryness, mechanical friction and wounding, hyper-osmolarity, temperature, wind or touch, is sensed and typically a respective answer is triggered in the brain stem in order to evoke responses that´solve the problem´.
The respective answer can be an increased glandular secretion or it can be an innervation of the lid muscle in order to trigger blinking, either for a protective eye closure or as a means to renew the tear film.
Eye closure, blinking and secretion are closely related and when the ocular surface is accidentally touched this typically results in eye closure and tearing, probably followed by blinking.
Pain is another function of the nervous system
Functions of the Nervous System are not only the regulation of the tissue function, as explained in the previous paragraph, but also the sensations and pain.
The NERVOUS SYSTEM is connected via afferent nerves (here interrupted blue lines) from the Ocular Surface and efferent fibers (here solid green lines) to the Peripheral Organs. Both fiber types have their center in the regulatory unit of the Brain Stem of the Central Nervous System. Functions of the Nervous System are not only the REGULATION of the tissue function in a neural reflex arcs via the cranial nerves V (trigeminal) and VII (facial) but also the Perception of Neural Sensations and of Feelings of PAIN.
Sensations mean that a stimulus comes into consciousness and is thus realized as a basically neutral information. The region for conscious realization of such external stimuli is the cortex - the outer grey layer of the brain.
Pain, in contrast, is not a ´simple´ incoming neural sensation but is typically associated with an emotional ´color´ of feelings that are typically negative.
The biological function of pain is to trigger an adverse reaction in order to avoid the (further) influence of a stimulus that endangers the integrity of the body. The region for the emotional ´coloring´ of neural inputs is deeper towards the center of the brain. A well known system associated with emotionalism is the limbic system that forms a circular arrangement of different structures that are all involved in emotions.
The emotional character and the severity of pain to a certain alteration of the ocular surface can therefore vary to a considerable degree in different patients and in different conditions. This may explain why there subjective pain feelings of a patient and objective clinical findings of a clinician can sometimes be disparate.
Chronic pain syndromes may also develop, so that the feeling of a pain may torture a patient without any too significant objective findings at the ocular surface. In such cases it can often become difficult for the patient and for his doctor to find suitable solutions for this bothersome situation.
=> here you can find more information on the Neural Regulatory System for Secretion, Blink and Pain
The organs of the ocular surface are all connected to the endocrine system of hormones. This concerns the circulation of hormones and hormone precursors in the blood stream that are of major influence for the growth, differentiation and functional regulation of the ocular surface.
Some elements of the Endocrine Hormonal System with respect to Sex Hormones are shown here schematically. The superior centers in the hypothalamus and pituitary gland regulate dependent glands such as the Adrenal Gland and the Gonadal Glands (Ovary and Testis). The prevailing amount of sex hormones is typically produced in peripheral tissues such as in the ocular surface organs (see diagram above). At present Sex Hormones appear to have the greatest influence on the Ocular Surface but other Hormones and soluble factors may also be of importance.
Of prime importance appear to be the sex hormones but numerous other soluble factors are also relevant. ´Male´ sex hormones (androgens) and ´female´ sex hormones (estrogens and progesterons) are actually present in both sexes - however in different proportions.
The sex hormones are in both male and female important for the growth and differentiation of the organs in development. The conjunctiva as well as the connected glands respond equally to the hormones. Much of the sex hormones are produced locally in the ocular tissues from hormone precursors in the blood.
In adulthood, the function of the ocular surface tissues and particularly of the glands seems to be more positively influenced by androgens in both sexes. This explains why females typically have a higher risk for Dry Eye Disease due to the lower level of androgens. Perturbations of hormone levels in menopause can further disturb the physiological function of the ocular surface.
Many bone marrow derived cells, that have typically spherical and rather dark nuclei, populate the loose connective tissue of the ocular surface organs together with blood vessels and nerves (figure A). They are basically leukocytes (white blood cells) and have protective functions against different sorts of negative influences including microbes etc. Fewer leukocytes (dark nucleus in figure B) occur In the overlying layer of densely aggregated epithelial cells (epithelium) that seals the tissue against the outer environment
The influence of the mucosal immune system is of longtime underestimated importance for ocular surface health and disease. This system is continuously present, as diffusely interspersed cells and lymph follicles in certain locations as reported over the years in several peer-reviewed articles in much detail by members of the Ocular Surface Center Berlin (OSCB). In the last about two decades increasing evidence was found for a distinct role of inflammation as an important amplification mechanism in ocular surface disease of the Dry Eye type.
Events in Inflammatory Mucosal Disease of the Ocular Surface are influenced by Dysregulation of the Mucosal Immune System with Inflammation and Onset of a Vicious Circle (large arrow, right)
There is a lot of evidence that inflammation appears leads to a dysregulation of the immune system - which then, in its deregulated state, can become a potent amplifier of inflammation from an innate sub-clinical inflammation into an immune-mediated one.
This similarly observed in other mucosal organs, such as in the intestine in ´Inflammatory Bowel Disease´ and is collectively termed as ´Chronic Mucosal Inflammation´.
The conceivable reason is, that mucosal organs typically have the opposing tasks to prefer tolerance against the prevailing vast majority of non-pathogenic antigens in order to avoid destructive unnecessary reactions whereas, on the other hand, the vigorous defense against pathogenic antigens has always to be at arms. When chronic inflammatory events then provide controversial signals to the immune system ... sometimes players in this intricate system ´become nervous and pull the trigger´ - an inherent danger to all highly alarmed systems.
The mucosal immune system of the Ocular Surface (Eye-Associated Lymphoid Tissue, EALT) is an important regulatory system for the Ocular Surface because it protects the moist and nicely temperatured Ocular Surface Niche against microbial infection. Chronic irritative stimuli, however, e.g. due to environmental stimuli, can induce inflammatory mediators that may lead to chronic inflammation. This can dysregulate the Mucosal Immune System in a way that immune modulated ocular surface inflammation can result in vicious circles and drive the disease process.
The previous observation that a local immune system with resident lymphoid and other immune cells is physiologically present at the normal ocular surface as well as deeper insight into the regulation of the mucosal immune system in other organ systems of the body has made it easier to understand how and why a dys-regulation of the physiologically protective system can occur and how this may transform the response to chronic noxes into a self-perpetuating disease process